By Codi Darnell
March 2, 2021

Lisa and Peter Marshall have a love story that spans 20 years. For eight of those years, they sustained a long-distance relationship so as not to disrupt their children’s lives – crossing states to see each other every weekend they could manage. Finally, in August of 2009, they said “I do” in Turks and Caicos with their five children by their side, and Lisa moved her life to Connecticut.
You only have to look at their photos to see the vibrancy between them. These self-described lovebirds found joy in simple things together: running, playing cards, spending time with their children, and whisking each other away for a weekend trip or a visit to the winery. But all that began to change in April 2018 when Peter, at 53 years old, was formally diagnosed with Alzheimer’s disease.
As Peter declined, Lisa took on the role of caregiver and, in May of 2019, began to share their journey on her Facebook page Oh Hello Alzheimer’s. Her stories are honest and thought-provoking. The love she has for her husband is evident in her compassion and patience, but she doesn’t hide the struggle or pain that comes from caring for someone – a partner – who is slowly disappearing. As she often says, “I miss my husband”.
I was able to connect with Lisa and get some of her thoughts on caregiving and Alzheimer’s disease.
What inspired you to start Oh Hello Alzheimer’s and share your journey publicly?
Peter was golfing – he was still able to participate in his men’s league then. I was spending a quiet evening at home alone, just me and Cabernet. I became very emotional and, honestly, needed some support. I wanted to scream “This is happening to us! Can you see this?”; I wanted someone to save us. I felt helpless and I was absolutely raging with fear, horror, sadness and grief, and I wanted everyone who would listen to know.
People needed to see and feel this tragic disease because no one talks about the real and raw experiences. Few allow themselves to be open and vulnerable in sharing their private and daily grief and desperation.
People need to understand that Alzheimer’s disease is not just memory loss, like “Where did I put my keys?”. This disease takes everything you are – every single thing – day by day, hour by hour.
Caregivers MUST have a resource for what could be coming, and I want to pave the way for them by sharing our journey – to help them guard their hearts and prepare their souls for the devastating grief of losing a young spouse while their body lives.
There is no handbook, and every case is different. But if I can help make a difference by creating awareness for caregivers about younger-onset Alzheimer’s disease and spreading kindness, I want to do just that.
You are Peter’s main caregiver. How did you decide that was the right choice for you?
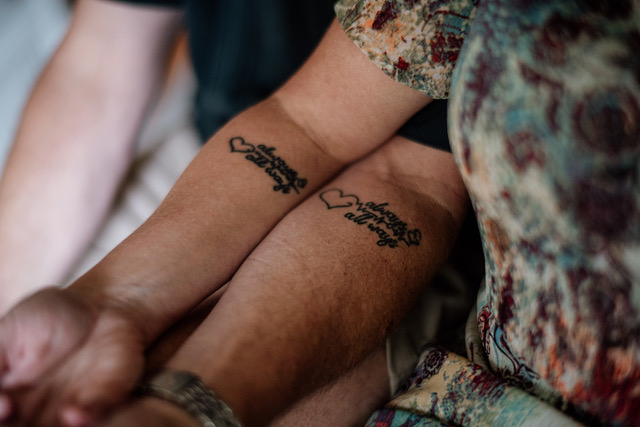
There was never a question of who would care for Peter. But at the time that I made the decision, I wasn’t looking at it through the eyes of a caregiver, I simply wanted to spend as much time with Peter as I could.
Many families are burdened with the need to continue working in order to be able to pay for care when the time comes. We were very fortunate that I was able to retire early and take on that caregiving role when I felt leaving Peter alone was no longer safe. I retired on December 31, 2019, at the age of 53. Peter was 54.
As Peter deteriorated, I could no longer manage caring for him alone. To say that it’s physically and emotionally exhausting is an understatement. I needed breaks to stay strong for him – to continue to be kind and patient. I now have caregivers that come in three times a week, four hours a day – this allows me 12 out of 168 hours off the clock per week. As he declines that will need to be stepped up to five days, and eventually seven days, for several hours each day. But, for now, this is manageable.
What advice do you have for someone who is starting their caregiving journey and dealing with a new diagnosis of a loved one?
Two critical pieces of advice come to mind. First and foremost, you must take care of yourself and find respite hours to try to shut off your mind. Someone once told me that if I didn’t continue to nurture myself, I’d be a shell of a person when this is over.
Most caregivers wait far too long – until they’re emotionally and physically drained – to start a regular self-care routine. Starting early not only protects the caregiver from burnout but helps the person with Alzheimer’s disease adapt to other caregivers. And isn’t that a precious gift to provide our loved one – several people that they can trust?
Secondly, not only should you accept help from the people who offer, but you should ask for it. You’ll hear frequently, “If there’s anything I can do let me know”. People want to help but they don’t know what a caregiver needs. If you need a prescription picked up, ask. If you need 30 minutes to take a walk, ask. If you need meals for your freezer, ask. Put yourself in their shoes of wanting to help but not knowing what to do. When we help others, we feel part of something larger. We feel useful and connected.
Friends and family have helped me move wood, clean my basement, sit with Peter while I get my hair done or go to the doctor. They’ve taken him sledding, running, to Build-a-Bear, to the aquarium, for walks and so on. Accept the offers and ask for help.
Catch yourself when you hear yourself saying, “No, I’m fine”, and change it to “YES, I could use a hand”.
You shared a story about shovelling the driveway. Can you tell us about that and what it’s been like to see the regular roles in your marriage shift?
Peter has always loved shovelling and would spend hours clearing snow. I would clean off the car. Our driveway is about five car lengths long and the snow was wet and heavy. I bundled Peter up and gave him a shovel and assumed the chore would be as it always had been. It was not.
I realized I was now the heavy lifter as Peter no longer remembered how to scoop and throw the snow to clear a path – not to the porch, not on the walkway, not on the driveway. As I took breaks for my aching back, I leaned on the handle of my shovel as my emotions ran the gamut from anger to resentment and self-pity. I was miserable and ready to spit nails when Peter sauntered towards me with a huge proud smile, kissed my face and asked me if I was okay, then announced with certainty, “You can do it!”
My heart swelled and I laughed at the irony. It was the motivation I needed to finish and the essential reminder that none of this is in his control. Thank goodness I was able to remain patient and kind long enough to make that sweet memory.
There used to be tasks and chores that I could ask Peter to do: take out the trash, get the mail, feed the dogs, bring down the laundry. He no longer understands the steps that need to be taken to complete these complicated duties. For instance, take out the trash has far more steps for Peter than for you or me. What is the trash? Where is the trash? How do I get the trash? What do I do with the trash? Where do I take the trash? Opening the door, finding the route to the trash can. Which receptacle?
I am responsible for every single household duty in our home now. Peter can sometimes still understand how to let the dogs in from outside. If I fill up his arms with wood for the fireplace, he will carry it. If I hand him the laundry, he will take it downstairs. We do everything together.
How do you balance caring for Peter and caring for yourself?

I’ve never been very good at balance, but I’m getting better the more I practice. It’s difficult to let go and allow someone else to take care of Peter – especially when he gets so anxious. Guilt gets in the way. I’ve always been a very independent and a strong individual and have an incredibly hard time asking for or accepting help, but I’m growing. Learning this valuable life lesson has taken a deliberate effort.
This guilt and stubbornness caused me to become out of balance: overwhelmed, exhausted, sad, resentful, even manic. Having a few hours on the calendar, a regular respite schedule intact, gives me some time to look forward to and strength to hang on a little longer. It helps to put a routine in place and make the time to take care of myself, even if its just reading a book in another room without being distracted.
There are 168 hours in a week, spouses sleep with one eye open to make sure our loved ones are safely tucked in. We tiptoe around the house to find where they snuck off to. We are always on.
What is balance anyway? I think it’s keeping my mind in a peaceful place to remain calm and ready for the next new normal which is always just around the corner. I know I’m out of balance when emotions like anger, resentment or impatience bubble up. That’s when I must stop and focus on self-care. Being proactive is a better plan – have a caregiving team in place instead of being reactive and trying desperately to find someone to help.
What do you want people to understand about Alzheimer’s disease and caregiving?
The most important thing is to make your loved one feel safe and loved, constantly. They are confused nearly all day; they feel inept and without purpose. Everything that surrounds them feels strange. They are frightened by things they see and hear that are not there. They are exhausted from pretending they know who people are and what everyone is talking about.
Can we all slow down and compassionately think about how THAT MUST FEEL.
Caregiving is exhausting, all consuming, rewarding, shocking, repulsive, worthy. It is relentless work. But if you do the work, and put a respite schedule in place for yourself, you can come out of this with no regrets. Be patient with your loved one, and equally important, be patient with yourself.
There are few options for financial help with younger-onset Alzheimer’s disease. Caregiver costs are on average $20 an hour with a 3-hour minimum. You want to have a cup of coffee with your friend? Need a mammogram? Need to go to the dentist? You’re paying $60 to walk out the front door. You’re paying out-of-pocket unless you have long-term care insurance, are a low income earner or on hospice.
So, for a caregiver to stay with Peter for three days, four hours a day, the average cost is $240 a week, nearly $1,000 a month. It’s expensive and this is a very minimal schedule. We’ll need a lot more care in the coming year.
